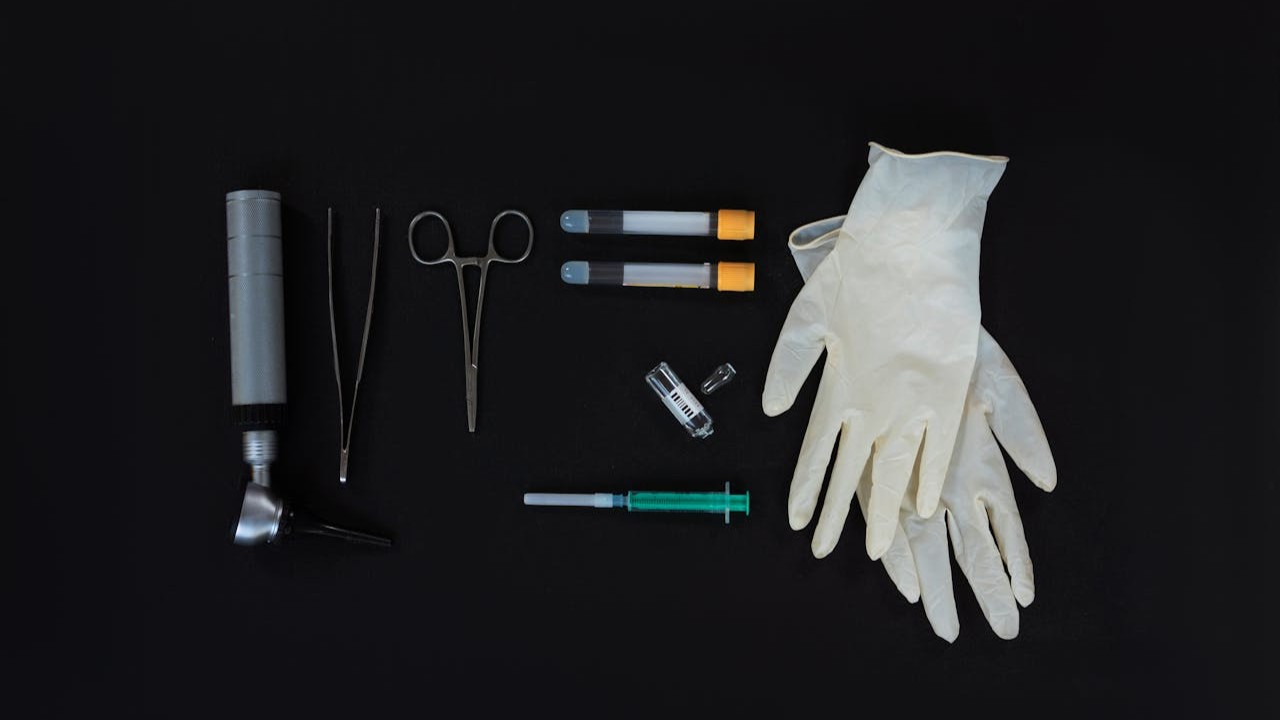
What the phrase really means?
Despite the nickname, it does not involve a kitchen baster. In practice, it means collecting fresh semen in a sterile, wide-mouth cup and placing it close to the cervix with a small, needle-free syringe. In clinical language, this is closest to at-home intracervical insemination, or ICI. If you want a direct comparison with clinic care, see the ICI guide.
What matters most?
- The fertile window is the few days before ovulation and the day of ovulation. NHS: how to get pregnant
- Well-timed attempts matter more than trying randomly throughout the cycle. NHS: infertility overview
- Simple habits help: do not smoke, keep alcohol sensible, maintain a healthy weight, and take folic acid before conception. NHS: vitamins and supplements
Safety and hygiene
- Use new, single-use syringes and a sterile collection cup. Avoid saliva and non-sperm-safe lubricants because they can reduce motility. HFEA: using donated sperm
- Use the sample within about an hour at room temperature, and keep hands and surfaces clean.
- Banked donor sperm is screened and handled under donor-eligibility rules. HFEA: donors and donation
Supplies checklist
- Sterile, wide-mouth collection cup
- Small needle-free medical syringe, usually 5 to 10 mL
- Ovulation predictor tests, either LH strips or digital tests
Optional: disposable gloves, a clean towel, and a lubricant labelled fertility-friendly. If you want a more structured setup, see the home insemination kit guide.
At-home steps most people follow
- Collect semen in the sterile cup without condoms or saliva.
- Let it stand at room temperature for 10 to 15 minutes so it can liquefy.
- Draw it up slowly and tap out air bubbles.
- Lie comfortably with hips slightly elevated. Place the syringe tip just inside the vagina and angle towards the cervix.
- Press the plunger gently and rest for 15 to 20 minutes afterwards.
Stop if anything feels painful or uncertain and contact a clinician.
Timing that helps
- Many people use LH tests to narrow the fertile window and aim for the first positive result or the next day. NHS: timing and ovulation
- The fertile window is short, so a simple timing plan is usually more useful than repeated guesswork. NHS
- Start folic acid before conception and keep the rest of the routine steady. NHS
Alternatives and how they differ
- Clinic IUI with donor sperm adds screening, consent, and medical oversight, and it places prepared sperm directly into the uterus.
- Timed intercourse with a partner uses the same fertile-window logic and is often the simplest first step before testing or treatment.
- If the bigger question is the overall treatment path, assisted reproduction can help you compare home insemination, IUI, IVF, and ICSI.
Legal basics you should know
Rules on known donors and legal parentage vary by country and sometimes by region. In the UK, private arrangements can still create parentage questions, so if you rely on a known donor, review the rules where you live and consider advice from a solicitor experienced in assisted reproduction.
If the arrangement is private, the private sperm donation guide covers testing, documentation, and the practical risks to plan for.
When home insemination is a reasonable fit?
- You have a cycle pattern that lets you estimate ovulation with some confidence.
- The donor arrangement is clear and the sample source is agreed in advance.
- You want a lower-tech first step while you wait for clinic care or testing.
- You are comfortable taking responsibility for hygiene, timing, and documentation.
It is usually a weaker fit when cycles are very irregular, there is known tubal disease, sperm quality is already a concern, or you need legal clarity that only a clinic-based process can provide.
When to see a clinician?
- Under 35 and not pregnant after 12 well-timed cycles
- 35 or older and not pregnant after 6 well-timed cycles
- Right away for very irregular cycles, suspected anovulation, endometriosis, PCOS, thyroid disease, recurrent pregnancy loss, or safety questions
Your clinician can help decide whether you need testing, a clinic-based insemination plan, or a different fertility treatment altogether.
Myths and facts
- Myth: A kitchen turkey baster works. Fact: it is unsafe and unsuitable, so a small medical syringe is the right tool.
- Myth: Any lubricant is fine. Fact: some lubricants reduce sperm motility, so fertility-friendly products are the safer choice. HFEA
- Myth: Legs-up guarantees success. Fact: timing around ovulation matters much more than a posture trick. NHS
- Myth: Home attempts remove legal risk. Fact: parentage rules differ by jurisdiction, so know them before you proceed. HFEA
Conclusion
Turkey baster pregnancy is slang for syringe-based attempts at home. If you explore this path, keep it clean and simple, time it around ovulation, and take the legal side seriously. If progress stalls or you want more certainty, speak with a clinician about testing, clinic IUI, or the next step that fits your situation.