Understanding PCOS
PCOS is a syndrome, meaning a cluster of possible features. It can affect ovulation and cycles, skin and hair growth, and metabolism, often through insulin resistance.
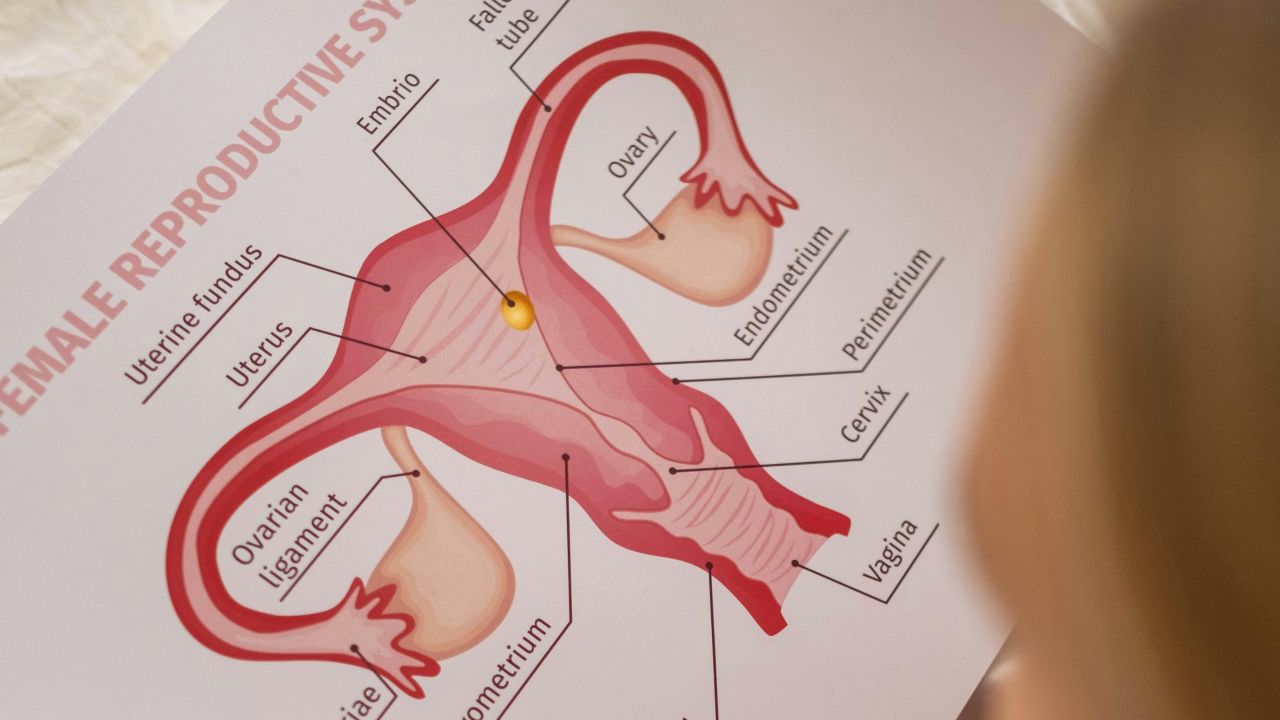
The name can be misleading. It usually is not about true cysts. On ultrasound, clinicians often see many small follicles, which are early egg follicles that may not mature all the way to ovulation in some cycles.
For context: PCOS is one of the most common hormonal conditions in people of reproductive age. The World Health Organization cites an approximate range of 8% to 13%. A clear starting point is the fact sheet: WHO on PCOS.
Which symptoms can fit PCOS?
PCOS is not one fixed picture. Some notice it mainly through their cycle, others through skin changes, and some only when trying to conceive or when blood tests are done. Common clues include:
- irregular bleeding, cycles longer than 35 days, or long gaps without a period
- rare or absent ovulation
- acne after puberty or persistent acne
- increased body or facial hair growth
- abdominal weight gain or weight that is hard to stabilise
- difficulty conceiving because timing is hard without regular ovulation
You can have PCOS without being overweight. Normal weight does not rule it out, and higher weight does not prove it.
Why does PCOS happen? A practical explanation?
The exact cause is not fully understood. Most evidence points to a combination of genetics and biological feedback loops that, in some people, shift toward higher androgens and insulin resistance.
In practical terms: when insulin stays high, it can support higher androgen production and disrupt ovulation. Androgens can influence skin and hair growth. Weight can amplify these loops, but it is not the root cause in itself.
The key point is this: PCOS is not a willpower problem. Lifestyle changes can be a powerful lever, but they do not explain everything.
Diagnosis in guidelines: which criteria are used?
For adults, many guideline pathways use three core elements. Often, PCOS is considered likely if two of the three are present and other causes have been excluded:
- irregular or absent ovulation
- clinical or biochemical signs of androgen excess
- an ultrasound pattern with many small follicles
The second part matters: some conditions can look similar and should be considered depending on your symptoms, for example thyroid disorders or elevated prolactin.
A patient-friendly explanation is available here: NHS on PCOS.
PCOS in puberty and adolescence
In the first years after the first period, irregular cycles are common even without PCOS. That is why guidelines recommend being cautious in adolescents. Often, the best approach is to identify risk and follow patterns over time rather than locking in a diagnosis too early.
What tests are typically part of a PCOS assessment?
There is no single PCOS test. The assessment usually combines history, an exam, and labs. The goal is to interpret the criteria, consider look-alikes, and catch metabolic risks early.
- history: cycle patterns, acne, hair growth, weight changes, pregnancy plans, medications
- physical exam: blood pressure, weight, signs of androgen excess
- labs: androgens, and often thyroid and prolactin depending on your case
- metabolic screening: blood glucose and lipids, especially if risk factors are present
- ultrasound: ovaries and, when periods are very infrequent, sometimes the uterine lining
The 2023 international evidence-based guideline also discusses anti-Müllerian hormone as an alternative to ultrasound in some adult settings, but not for diagnosis in adolescents. The summary publication is here: International PCOS guideline 2023.
Long-term risks: why follow-up matters
PCOS is not only a fertility topic. Guidelines highlight that PCOS can affect overall health. Long-term, the focus is often on:
- insulin resistance, impaired glucose tolerance, and type 2 diabetes
- high blood pressure and lipid abnormalities
- sleep apnoea, especially when risk factors are present
- pregnancy complications such as gestational diabetes and hypertension
- a higher risk of endometrial changes when periods are very infrequent or absent
This does not mean you will automatically develop severe complications. It means smart follow-up helps catch issues early and prevent escalation.
Typical follow-ups include blood pressure, blood glucose, and lipids, plus a clear plan for regular bleeding if periods are rare. The right interval depends on your risks and life stage.
Diet and exercise: the foundation, without extremes
Lifestyle is a core recommendation in many guidelines. It does not replace medical care, but it can strongly support it. What matters is not a perfect plan, but one you can sustain.
- eat in a blood-sugar-friendly way: vegetables, legumes, whole grains, nuts, and healthy fats, with fewer sugary drinks and ultra-processed snacks
- move realistically: endurance plus strength training is a strong combination, including at normal weight
- take sleep and stress seriously: both influence appetite, insulin, and cycle regulation
If you feel overwhelmed, start deliberately small and make it stable.
Medications in PCOS: a clear overview
PCOS rarely comes down to one medication. Instead, treatment is built from components. Broadly, these areas are common:
- cycle regulation and androgen symptoms: often hormonal contraception when you are not trying to conceive
- metabolic features: metformin is commonly used when metabolic issues are a priority
- trying to conceive: ovulation induction medications with monitoring
Supplements are widely discussed, but not all options have the same evidence. If you use them, be clear about your goal and how you will measure benefit.
Treatment when you are not trying to conceive
If pregnancy is not the goal right now, many people focus on cycle management, skin symptoms, and long-term risks. Guidelines often list combined hormonal contraception as a first option for cycle control and androgen symptoms.
When periods are very rare, the goal is also to protect the uterine lining. Which option fits best depends on medical risks, tolerability, and contraception preferences.
If you want a quick overview, guideline summaries and major health resources are usually more helpful than social media anecdotes.
Treatment when trying to conceive
When trying to conceive, a structured plan helps. Many people with PCOS conceive spontaneously, others benefit from support, especially when ovulation is absent.
1. Make ovulation easier to interpret
If you want to know whether and when you ovulate, temperature charting and ovulation tests can be a good starting point. With PCOS, it often helps to look at patterns over time rather than one isolated strip. Background articles are here: Ovulation and LH tests.
2. Do not forget other factors
Even with PCOS, it is worth checking semen parameters and tubal patency when appropriate. This helps avoid focusing on one lever while other factors are present.
3. Ovulation induction
When ovulation does not happen, medications can be used to trigger it. The 2023 international evidence-based guideline names letrozole as the preferred first pharmacologic option. Other routes include clomiphene, sometimes combined with metformin, and then gonadotropins with close monitoring.
For a clearer overview, see ovarian stimulation.
4. When medications are not enough
If ovulation induction is not successful or other factors are involved, further options may be appropriate, for example in vitro fertilisation, often shortened to IVF. Depending on the situation, intracytoplasmic sperm injection, often shortened to ICSI, may also be discussed. With PCOS, the risk of ovarian hyperstimulation is higher, so careful protocols and monitoring matter.
If you are pregnant or planning to be, it is also worth watching metabolic factors and blood pressure, because PCOS can be linked to higher risks of gestational diabetes and hypertension. That does not mean complications are inevitable, it means preparation and follow-up are especially useful.
One reassurance: PCOS changes over time. In some phases it is mainly about cycles and skin, later it may be more about metabolism and follow-ups. Your plan can evolve with you.
Acne, hair growth, hair loss: practical steps
Many people want visible improvements first. That makes sense, because these symptoms can be hard in daily life. Common components include:
- treating the hormonal drivers when appropriate for your situation
- dermatology care for acne
- mechanical hair removal or laser options for excess hair
- patience: hair growth and hair loss often respond slowly, not within days
If you notice very sudden or rapidly worsening androgen symptoms, timely medical assessment is important.
Mental health: a central part of PCOS
PCOS can be psychologically stressful because body image, skin, hair growth, weight, and fertility can create pressure. Guidelines emphasise that depressive symptoms and anxiety are more common and should be taken seriously. If PCOS is taking up too much space in your head for too long, that is not a personal failure, it is a signal to actively plan support.
Myths and facts about PCOS
- Myth: PCOS means you have true cysts. Fact: often it is many small follicles rather than classic cysts.
- Myth: PCOS only happens with overweight. Fact: PCOS can exist at normal weight.
- Myth: without a regular cycle, pregnancy is impossible. Fact: many conceive spontaneously or with support.
Appointment checklist
If you feel like you are bouncing from appointment to appointment, three questions often help more than a long list:
- Which criteria support PCOS in my case, and which do not?
- Which alternative causes should be considered for my pattern?
- What are the next two steps for me right now?
Conclusion
PCOS is common and can be very stressful, but it is treatable. What helps most is an individualized plan that connects cycles, skin, metabolism, and your life stage, with smart follow-ups and clear next steps if you are trying to conceive. With guideline-based assessment, sustainable lifestyle basics, and the right medical options, many people see meaningful improvements in quality of life.